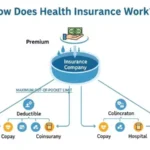
Understanding can insurance cover massages is important for anyone looking to reduce the cost of massage therapy for pain relief or wellness care. Many health plans offer coverage for medical massage, therapeutic treatment, and doctor-recommended massage sessions, but the rules and eligibility vary. Knowing how insurance providers verify medical necessity, what documentation they require, and which massage therapies qualify can help you save money and get the right care. Let’s explore how massage coverage works and what you should expect from your plan.
Can Insurance Cover Massages

Many people ask can insurance cover massages when they are considering massage therapy for health benefits. The short answer is yes in certain situations, especially when massage is part of a treatment plan prescribed by a doctor for medical conditions. Most health insurance plans do not cover general wellness massage, but medical massage therapy or therapeutic massage may be covered if you meet specific criteria. To qualify, you usually need:
- A referral or prescription from your healthcare provider
- Clear documentation showing medical necessity
- Treatment by a licensed massage therapist
- Your plan’s prior authorization or pre-approval
Insurance coverage varies widely between health plans, so always check your specific policy benefits and exclusions before scheduling sessions.
Can Insurance Cover Massages for Back Pain
Many individuals seek relief from chronic back pain through massage therapy, so it is important to understand how insurance handles coverage for this condition.
When Back Pain Massage May Be Covered
Massage therapy for back pain may be covered by insurance if:
- Your healthcare provider documents chronic back pain and prescribes massage as part of a treatment plan
- The massage therapist is licensed and recognized by your insurance provider
- You have a treatment plan with measurable goals for your back condition
- Sessions are coded correctly with medical billing codes such as CPT or ICD-10
What Insurers Typically Require
- Physician referral or recommendation
- Clinical notes showing improvement over time
- Pre-authorization from your insurance plan
Back Pain Massage Coverage Table
| Requirement | Why It Matters |
| Doctor referral | Confirms medical necessity |
| Licensed therapist | Ensures provider eligibility |
| Pre-authorization | Prevents claim denial |
| Medical billing codes | Correct processing by insurers |
In summary, massage for back pain may be covered if it is medically necessary and part of an approved treatment plan.
Can Insurance Cover Massages for Seniors
Seniors often benefit from massage therapy for conditions like arthritis, muscle stiffness, and circulation issues. Can insurance cover massages for seniors depends on the type of insurance and how the massage is used in the treatment.
When Coverage Is Possible
- Senior has a doctor’s order for therapeutic massage
- The treatment addresses conditions such as arthritis pain, post-surgery recovery, or mobility improvement
- Massage is part of rehabilitation therapy under Medicare Advantage or supplemental plans
Typical Requirements
- Clear medical record of symptoms and treatment goals
- Provider credential validation in the plan’s network
- Proper medical billing and claim submission
Seniors should always confirm with Medicare Advantage, Medigap, or private health insurance what documentation is required for coverage.
Massage Covered by Insurance Blue Cross Blue Shield
Blue Cross Blue Shield (BCBS) is one of the major insurance providers in the United States. Many BCBS plans may offer coverage for massage therapy under certain conditions.
What BCBS Typically Covers
- Therapeutic massage for specific medical diagnoses
- Treatments included in a rehabilitation program
- Services provided by licensed and credentialed therapists
Important Points
- Coverage depends on your specific BCBS policy and state regulations
- A doctor’s referral or treatment plan is often required
- Sessions may require pre-authorization before insurance will pay
Always review your individual BCBS member handbook or contact customer service for the most current coverage details.
Can Insurance Cover Massages in Florida
Insurance coverage for massages in Florida follows the same general rules as the rest of the United States, but state regulations and plan differences can affect what is covered.
Florida Specifics
- Florida insurers may follow state healthcare requirements for medical necessity
- Many plans require a physician’s prescription for therapeutic massage
- Coverage may vary between commercial health plans, Medicare Advantage plans, and Medicaid managed care
Coverage Tips for Florida Residents
- Ask your doctor to provide a detailed treatment plan for massage therapy
- Verify that your massage therapist is licensed in Florida
- Confirm with your insurer whether pre-approval or prior authorization is needed
If you are in Florida and wondering can insurance cover massages in Florida, it is best to contact your plan directly for up-to-date information based on your coverage.
Deep Tissue Massage Covered by Insurance
Many people ask if deep tissue massage is covered by insurance, especially when they need targeted relief for muscle tension or injury recovery. Insurance may cover deep tissue massage when it is classified as medical massage therapy and prescribed by a doctor to treat a diagnosed condition. General relaxation or stress-relief massage is usually not covered.
When Deep Tissue Massage May Be Covered
- You have a documented medical issue such as chronic pain, muscle strain, or post-injury stiffness
- A doctor prescribes deep tissue massage as part of a treatment plan
- Your therapist is licensed and approved by your insurance provider
- Sessions meet the medical necessity criteria set by your plan
Important Factors Insurers Check
- Diagnosed condition
- Treatment goals and progress notes
- Frequency and duration of sessions
- Proper medical billing codes
If all requirements are met, your plan may partially or fully cover the cost of deep tissue massage.
Does Aetna Insurance Cover Massage Therapy

Aetna offers coverage for massage therapy when it is medically necessary and part of prescribed treatment. Aetna does not typically cover massages for wellness, relaxation, or personal comfort.
What Aetna Usually Covers
- Therapeutic massage recommended by a physician
- Massage included in a physical therapy or rehabilitation program
- Sessions performed by licensed and credentialed providers
- Treatment linked to conditions like back pain, injury recovery, or musculoskeletal disorders
What Aetna Usually Does Not Cover
- Spa massages
- Relaxation massages
- Non-medical massage packages
Helpful Tips
- Always ask your doctor to document your condition clearly
- Verify if prior authorization is required
- Keep detailed receipts and session notes for claims
Aetna’s coverage varies by state and plan type, so checking your policy details is essential.
How Much Does Insurance Pay for Massage Therapy
The amount insurance pays for massage therapy depends on the provider, diagnosis, and your specific insurance plan. Coverage typically ranges from 40 to 100 percent of the allowed amount when medically necessary.
Typical Coverage Scenarios
| Coverage Type | Average Payment | Notes |
| Full coverage | 80 to 100 percent | Usually with strict medical necessity evidence |
| Partial coverage | 40 to 70 percent | Most common for therapeutic massage |
| No coverage | 0 percent | Applies to wellness or relaxation massage |
Factors That Affect Payment
- Type of insurance (private, employer, Medicare Advantage)
- Deductible and copay structure
- Out of network vs in network therapists
- Frequency limits (example: 6 to 12 sessions per year)
To know exactly how much insurance will pay, check your plan’s benefits, allowed amounts, and required documentation.
Does Medicaid Cover Massage Therapy
Coverage for massage therapy under Medicaid varies by state. Most state Medicaid programs do not cover massage for general wellness, but some may cover medical massage when it is part of a treatment plan and recommended by a healthcare provider.
When Medicaid May Cover Massage
- Massage is included in treatment for medical conditions such as chronic pain or injury
- A physician or specialist documents the need for therapeutic massage
- The therapist is licensed and accepts Medicaid in your state
- Medicaid managed care organizations approve the treatment
State Differences
Some states offer limited coverage under rehabilitation or integrative care programs. Others may follow stricter rules and require strong medical documentation before approving any sessions.
Always check your state’s Medicaid guidelines or contact your plan administrator for the most accurate information.
Can Health Insurance Cover Massages
Many people want to know if health insurance can cover massages, especially when they need therapy for pain management or injury recovery. Health insurance can cover massage therapy when it is deemed medically necessary and recommended by a healthcare provider.
When Health Insurance Covers Massage
- You have a clinical diagnosis such as chronic back pain, neck stiffness, or soft tissue injury
- A licensed provider performs the massage
- Your plan allows therapeutic or medical massage benefits
- Proper medical records and billing codes are provided
What Health Insurance Usually Requires
- Physician referral
- Documented treatment plan
- Progress notes and follow up reports
- Pre authorization in some plans
Health insurance typically does not cover general relaxation or spa massages. Coverage applies mainly to medically necessary therapeutic sessions.
Can My Insurance Cover Massages
Many people wonder can my insurance cover massages when they are dealing with chronic pain, stress, or injury recovery. Most insurance plans will cover massage therapy only when it is labeled as medically necessary and prescribed by a healthcare professional. Wellness or relaxation massage is usually not included in standard coverage.
When Your Insurance Might Cover Massage Therapy
- You have a medical diagnosis that requires therapeutic massage
- A licensed doctor writes a referral or prescription
- Sessions support a treatment plan for conditions like back pain or muscle strain
- Your massage therapist is licensed and eligible under your plan
Before scheduling your sessions, review your insurance policy to understand your coverage, limits, and requirements.
Can You Get Insurance to Cover Massages
If you are asking can you get insurance to cover massages, the answer depends on how you plan your treatment. You can often get coverage approved when you follow the correct steps and meet your insurer’s medical necessity rules.
How to Get Insurance Approval
- Visit your doctor for an evaluation
- Request a written treatment plan recommending therapeutic massage
- Make sure the massage supports recovery from a specific medical condition
- Provide documentation such as progress notes and diagnosis codes
- Use an in network provider if your plan requires it
These steps significantly increase your chances of getting massage therapy covered.
Can Insurance Cover Prenatal Massages
Many expectant mothers ask if insurance can cover prenatal massages, especially when dealing with back discomfort, swelling, or pregnancy related tension. Prenatal massage is sometimes covered, but it depends on your insurance plan and your doctor’s recommendation.
When Prenatal Massage May Be Covered
- Your obstetrician or healthcare provider recommends it for medical reasons
- You are experiencing pregnancy related pain such as sciatica, muscle strain, or circulation issues
- Your provider documents the need clearly in your medical file
- The therapist specializes in prenatal massage and is licensed
Important Points for Pregnant Women
- Insurance rarely covers prenatal massage for relaxation
- Some plans cover it under maternal health benefits when medically justified
- Always check your provider’s prenatal care policy
If prenatal massage improves your health during pregnancy and your doctor supports it, coverage may be possible.
Can Your Insurance Cover Massages
The question can your insurance cover massages depends on how your plan defines medical necessity and what types of therapy are included in the benefits. Many insurance companies provide partial or full coverage for massage therapy when it supports treatment for an injury or health condition.
What Your Insurance May Cover
- Therapeutic sessions for chronic pain
- Post injury rehabilitation massage
- Treatment for musculoskeletal disorders
- Doctor prescribed medical massage
Coverage Requirements
- Physician referral
- Medical justification
- Licensed therapist
- Correct billing documentation
Understanding your plan benefits and following proper steps can help you get your insurance to cover the massages you need.
Can Medical Insurance Cover Massages
Many people want to know if medical insurance can cover massages when they need relief from chronic pain, injury recovery, or muscle tension. Medical insurance may cover massage therapy when the treatment is considered medically necessary and prescribed by a licensed healthcare provider. This means the massage must support recovery from a diagnosed medical condition, not just relaxation.
When Medical Insurance Usually Covers Massage
- Your doctor recommends massage as part of a treatment plan
- You have a documented diagnosis such as back pain, soft tissue injury, or muscle disorder
- The therapist is licensed and approved by your insurance
- The sessions aim to reduce pain, improve mobility, or treat a clinical condition
What Medical Insurance Does Not Cover
- Spa or relaxation massage
- Massage for stress relief only
- Sessions without medical records or treatment plans
Understanding your medical plan and following proper steps can help you verify what is covered.
How Can I Get My Insurance to Cover Massages
If you are asking how can I get my insurance to cover massages, the process is easier when you follow the insurer’s medical requirements. Most insurance companies need proof that the massage is not for wellness but for a medical condition.
Steps to Get Your Insurance to Cover Massage Therapy
- Get evaluated by a doctor
Your doctor should diagnose the condition and confirm that massage therapy will help. - Request a written treatment plan
This includes the reason, number of sessions, and expected improvements. - Use a licensed massage therapist
Insurance companies only reimburse sessions from credentialed providers. - Check pre authorization rules
Some plans require approval before your sessions begin. - Keep documentation
Progress notes, provider notes, and receipts help avoid claim denials.
Helpful Tips
- Ask your doctor to specify medical necessity clearly
- Verify session limits and allowed amounts
- Stay within network if your plan requires it
Following these steps greatly increases your chances of getting insurance coverage for massage therapy.
Does My Insurance Cover Massage
If you are unsure does my insurance cover massage, the answer depends on your policy type and medical needs. Many insurance plans cover therapeutic or medical massage when it is part of a documented treatment plan.
How to Check Your Coverage
- Review your insurance benefits section for therapeutic services
- Contact customer support and ask about medical massage therapy coverage
- Confirm if your plan requires a referral or prescription
- Check if your therapist must be in network
What Coverage Usually Includes
- Massage for injury recovery
- Treatment for chronic pain conditions
- Sessions that support physical therapy or rehabilitation
- Massage performed by licensed professionals only
Quick Coverage Table
| Coverage Status | What It Means |
| Likely covered | Medically necessary therapeutic massage |
| Sometimes covered | Massage linked to rehabilitation therapy |
| Not covered | Spa or relaxation massage |
Knowing your insurance benefits and understanding coverage requirements will help you determine whether massage therapy is included in your plan.
Frequently Asked Questions
Can insurance cover massages for pain relief
Insurance may cover massages for pain relief when a doctor confirms medical necessity and the treatment supports your recovery plan.
Does health insurance pay for massage therapy
Health insurance may pay for massage therapy if it is prescribed for a diagnosed condition and performed by a licensed therapist.
Can insurance cover massages for back pain
Massage for back pain is often covered when your provider documents the condition and recommends therapeutic sessions.
How do I get my insurance to cover massages
You need a doctor referral, medical documentation, and an approved treatment plan to get insurance to cover massage therapy.
Can medical insurance cover therapeutic massage
Medical insurance can cover therapeutic massage when it is part of a physician guided treatment plan for clinical issues.
Is massage therapy covered by insurance plans
Some insurance plans cover massage therapy when it supports treatment for chronic pain, injury recovery, or musculoskeletal problems.
Can insurance cover massages for seniors
Insurance can cover massages for seniors if a healthcare provider prescribes them to address pain, mobility issues, or rehabilitation needs.
Does insurance cover prenatal massages
Prenatal massage may be covered only if your doctor recommends it for health related pregnancy conditions and documents medical necessity.
Can insurance pay for deep tissue massage
Insurance may pay for deep tissue massage when it is required for treating muscle injuries or chronic pain with proper clinical documentation.
Will my insurance cover medical massage
Your insurance may cover medical massage if the sessions are tied to a diagnosis, treatment plan, and performed by an eligible provider.
Final Words
Understanding Can Insurance Cover Massages helps you make informed decisions about your healthcare options and treatment costs. When massage therapy is medically necessary and well documented, many insurance providers offer partial or full coverage, especially for chronic pain, injury recovery, and therapeutic care.
To benefit fully, always check your plan details, request proper referrals, and use licensed massage therapists. With the right documentation and provider guidance, Can Insurance Cover Massages becomes a practical and cost saving option for many individuals.

Chriselle Lim is a passionate digital creator and lifestyle blogger based in California, USA. As the voice behind Blogzeno, she shares creative captions, inspiring Instagram bios, insightful celebrity stories, and simple insurance guides designed for everyday readers. Emily believes that words have the power to connect people whether it’s through a perfect caption or a helpful article.
With years of experience in online writing and content strategy, Emily’s mission is to make information both useful and enjoyable. Her work blends creativity with clarity, helping readers express themselves confidently and stay informed about what truly matters.
When she’s not writing, you’ll find her exploring photography, social media trends, and new ways to inspire digital creators worldwide. Follow her journey on Blogzeno — where creativity meets everyday life.